Pelvic Health & Orthopedic Physical Therapy
Addressing your questions about pelvic, women's, and musculoskeletal health. Health is a journey. Movement is healing!
|
So pretty neat, more studies are being performed looking at pelvic floor training for overactive bladder. One study I came across this morning was recently published in the American Journal of Physical Medicine & Rehabilitation. I'll post the link I found below, but to summarize the findings they looked at pelvic floor training for Overactive Bladder (OAB) and urinary incontinence in two groups of women. One with idiopathic cause of symptoms. One group who had been diagnosed with Multiple Sclerosis. The researchers were monitoring the activity of the detrusor, the muscular layer inside the bladder. With their standardized exercise protocol almost half the women with idiopathic cause and about a fourth of the women with MS showed elimination of detrusor overactivity. So what does all that mean?
The bladder is a muscle. It has muscle on the outside, muscle on the inside. These muscles give and get information from the nervous system. The muscles of the bladder are also impacted by tissues around it like the pelvic floor muscles. There are certainly a lot of factors that can contribute to overactive bladder and incontinence. The link between the muscles of the bladder, the pelvic floor muscles (which are further south), and the nervous system play a large role. Proper use and implementation of urge suppression techniques suggested in this study can be helpful in hitting a reset to the system. A pelvic health physical therapist can help to assess and instruct individuals in proper urge suppression, as they were also part of this study. Essentially utilizing your pelvic floor muscles (which you can control), sends a message to the muscles of the bladder, which relays through the nervous system and brain to decrease the overwhelming urinary urge. Pretty awesome use of our voluntary nervous system! Study summary can be found here: https://www.sciencedaily.com/releases/2018/10/181019120736.htm Full journal: https://journals.lww.com/ajpmr/Abstract/publishahead/The_effect_of_pelvic_floor_muscle_contraction_on.98382.aspx One of my biggest pet peeves as a pelvic health PT is when runners or weight lifters think they need to leak urine to prove a good work out. Ugh! First of all it's gross. Second of all we don't see a problem with having an accident? If you are peeing unintentionally during any activity which does not include you sitting on a toilet you should see a pelvic and women's health physical therapist. Let me explain why.
The abdominal cavity has four sides to it. The top is the diaphragm. The front is the abdominal wall. The back is the spine and back musculature. The bottom is the pelvic floor. When you leak urine with exercise it indicates to me that something in this system is not operating to its best ability. In fact there may be more than one thing. Urine leakage generally indicates pelvic floor weakness. Weakness in this area means that one key aspect to the "core" is not optimally functioning. When we take a closer look what a pelvic and women's health physical therapist may find is that other aspects of the abdominal cavity are working less efficiently or compensating due to lack of coordination with pelvic floor musculature. Okay, okay you don't leak all the time. Just after the 10th mile on the pavement. Or just when you hit your rep max with dead lifts. This is still something we can work on. Yes it could still be a deficiency in pelvic muscle strength or endurance. It could be that the force of running on pavement or your form as you start to tire change your ability to activate pelvic floor muscles. It could be you don't even realize you are holding your breath with lifting which creates increased pressure on the bladder. So the moral of the story remains the same. You still should not accept urine leakage with exercise. A pelvic health physical therapist can help assess and treat this type of urine leakage and improve your work outs. The abdominal cavity is made up of four distinct borders. The top is the diaphragm, the back is the muscles of the back, the front is the abdominal muscles, and the bottom is compromised of the pelvic floor musculature. The abdomen contains a pressure system in this cavity which is influenced by our breathing and the activities we do throughout the day. This pressure is called "intra-abdominal pressure".
Intra-abdominal pressure can increase when you lift something, cough, sneeze, step down the stairs, and go from sitting to standing. Additionally, this pressure can change when you use the toilet if you strain. I mean think about it, have you ever tried to lift something heavy like a piece of furniture? Instinctively if something is really heavy we hold our breath to try to make the abdominal cavity stronger to lift the item. When we implement this technique we utilize pressure to press out against all borders of the abdominal cavity. Here's the catch it's can have some not so positive outcomes on our body. This increase in pressure presses right on your uterus, bladder and intestines (if you are a woman). These organs respond by going to areas of least resistance, the vaginal vault or rectal opening. This can contribute to pelvic organ prolapse. Additionally, it can cause the bladder to feel an increase in urinary urgency or may cause some accidental leakage of urine. It may also make an existing diastasis recti more challenging to deal with as you cannot appropriately generate force through your abdominal muscles. The number one thing to remember, DON'T HOLD YOUR BREATH. Don't hold your breath with lifting, don't hold your breath during exercise, don't hold your breath on the toilet. The next step is appropriately coordinating your breath, but never forget the number one rule. It is important to brace your pelvic floor and abdomen appropriately with more strenuous activity. If you feel that managing intra-abdominal pressure is something you find challenging you should see a pelvic health physical therapist. Happy Valentine's day! While you may be getting ready to spice things up with your partner don't forget to grab a good lubricant. Lubrication is key to an enjoyable intimate experience for you and your loved one. The female body produces a natural lubricant with stimulation and proper foreplay. Sometimes though it just isn't enough. This can be the case after menopause. Women stop producing estrogen after menopause and that natural lubrication system just doesn't work as well.
So on this day celebrating love and intimacy make sure you take care of your lady parts. In terms of lubricants you want to steer clear of petroleum based products like KY and things with a laundry list of chemicals. Your vagina has a microbiome of bacteria that can be irritated by the use of these types of products. You want to try to get a water-based lubricant. Brands include: Slippery Stuff, Sylk, and Blossom Organics. These can be purchased mostly online through your drugstore or Amazon. Additionally, you can utilize coconut oil for lubrication. However it CANNOT be used with condoms as it can break them down. So if this is your primary form of birth control look at a water-based product instead. If you are continually experiencing vaginal irritation and/or dryness throughout the day or pain with intercourse make sure to discuss that with your physician. Recently I was on Twitter and I saw a woman discussing the lack of postpartum care she received. It was distressing to say the least, but not necessarily unique. In fetal-maternal medicine most of the resources and focus are geared towards the baby. Even after giving birth the focus is on the new bundle of joy. Which is contributing to the rising rate of complications leading to death of mothers in the United States. Now fortunately this individual was very well educated in terms of her health, she seemed to advocate for herself and knew she needed to see a women's health/ pelvic PT. Unfortunately the one in her rural area was out on maternity leave. Thus she could not get the care she needed.
Most of the time women feel that the symptoms they experience postpartum are "normal" or they are embarrassed to talk about them so they don't share them with their OB/GYNs. Their OB/GYN may not even ask about symptoms of diastasis recti, urinary incontinence, organ prolapse, constipation, fecal incontinence, or pelvic pain at their check-up. If you are feeling symptoms of any of these things ADVOCATE for yourself! You know your body best! There is help out there. No one will know what is going on if you don't speak up and tell someone and then push for the services you want. Now here is my second soap box. The specialty of women's health and pelvic physical therapy is the second smallest specialty in the field of PT. This means that in some parts of the country, usually in more rural areas, there are no health care providers that treat individuals with these conditions. They are not trained to. Personally I have patients that travel over an hour to a few hours every week to get treatment and that is just unacceptable. We need more current and future PTs to be trained and treat men, women, and children with pelvic floor dysfunction in all parts of the country. There is no reason that individuals can't get care because they have to drive a few hours away every week. That is a large burden! If you feel that you require pelvic floor or women's health PT services please check these two databases for providers in your area. Just as an aside, not all clinicians may be listed as they must add their names to the list so I would also do a google search and ask your doctor if they know anyone locally before referring you to a different area. https://pelvicrehab.com/ http://www.womenshealthapta.org/pt-locator/ You went to the bathroom an hour ago, now you have to go again. In twenty minutes you will have to go to the bathroom once again. You will desperately need to find a restroom. Your life revolves around frequenting the bathroom to urinate, but when you go it doesn't always seem like all that much urine.
Does this sound like you? You may be experiencing the symptoms of overactive bladder. Individuals with this typically urinate more than eight times a day. When they do need to use the restroom, they are overcome with an intense urge to urinate. The urge make even lead to some urine leakage at times. When you do get to the restroom you quickly empty your bladder and head about your business, just to quickly rush back to the bathroom shortly. Why does this happen? Sometimes there is an underlying medical reason, other times we develop poor bladder health and train our bladder to go more often.So what can you do? A good first step if you suspect you have overactive bladder is to visit your physician. They can start medical management such as medications if necessary. You may also get referred to Physical Therapy to work on your pelvic floor muscles and retraining the bladder and your current bladder habits. Have you heard of painful bladder syndrome sometimes it's referred to as interstitial cystitis (IC)? It can be really tricky to diagnose so it could be years before getting diagnosed properly and receiving the right treatment. Some individuals just think they are continuing to get UTI’s even though the tests are negative. What is IC exactly? Even the definition is a bit tricky. The thought is interstitial cystitis is result of the lining of the bladder not functioning properly so the acidic contents of the bladder irritate the bladder wall. The body goes into an overdrive mode stimulating an inflammatory response and increasing the chemicals that make your body experience pain. The reason this occurs is not fully understood. Some studies point to genetic reasons, others say its root is in multiple bladder infections like UTI’s. When the organs have this reactions they have an effect on the musculature of the pelvic floor coupled with the pain that is experienced which leads to overactivity and tight musculature.
When the body develops this response it can either happen over a long amount of time or quickly. It is a painful syndrome, but can fluctuate in nature. So you will go through times of feeling okay and then times of intense pain. Pain is usually worse when you have a full bladder and is in the pelvic region primarily, but can occur elsewhere. You also may experience the need to get up during the middle of the night to use the bathroom. You might feel like you have to use the restroom more often or when you have to go you REALLY have to go! Pain may get worse around the time of your period. You may have pain with intercourse and following intercourse for a few days. If you feel like you are experiencing these symptoms and haven’t been treated the best place to start would to seek an appointment with a urologist or urogynecologist. They will run some tests to verify what is going on, help to get you on the correct medications, and possibly refer you to Pelvic Physical Therapy. There are a lot great websites out there with information. Here are just a few to start finding more resources. https://www.ic-network.com/ https://www.ichelp.org/ http://www.ic-today.com/ https://pelvicpain.org/home.aspx Do you ever laugh so hard a little pee just leaks out? Or maybe you are a cross-fit athlete and every time you do a lift you just leak a few drops. You just had a baby a few years ago and you never felt quite the same and now you notice when you gotta go to the bathroom you better start running or you end up with a little urine running down your leg. Maybe you constantly wear a pad or carry around extra panties due to fear of an accident.
Try as you might, you lose a little bit of pee, maybe it's even more than a small amount. This is called "urinary incontinence" when you unintentionally lose urine and there are a few different types. Stress Incontinence is when you accidentally lose pee. It can be with certain activities like coughing, sneezing, laughing, running, or when you stand up for sitting in a chair. These types of activities can change the pressure in your abdomen which influences your bladder and pelvic floor. If the muscles of your pelvic floor are weak they may have a difficult time staying closed to stop urine from coming down that urethra we talked about in the previous post. Urge Incontinence is when you accidentally lose urine with a strong urge to use the restroom. So you feel like you have to go to the bathroom and with the urge you lose control of your bladder and have a leak. The bladder has trained itself that it's time to go so you cannot wait. Oftentimes this is a mixture of pelvic floor musculature being both tight and weak. Functional Incontinence is when you physically cannot make it to the restroom so you have leakage. This could be that you are bed bound, unable transfer to the toilet on your own, or unable to unbutton your pants due to issues with dexterity in time causing loss in urine. So when does incontinence occur? Different types of incontinence can occur throughout different stages of life or with different conditions. Women commonly develop incontinence after giving birth and/ or after menopause. This can be due to the pelvic floor musculature going through changes as well as changes in hormones. And despite being told that this is "just old woman bladder" there is definitely techniques Physical Therapists can help you implement to better control your bladder. For men urinary incontinence and urgency can develop in individuals who have their prostate removed. 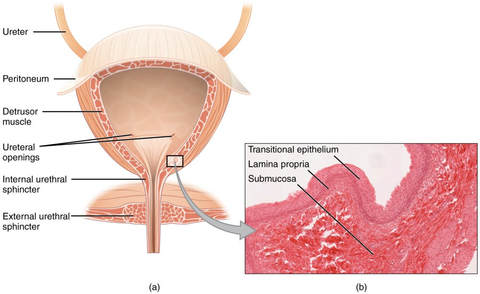 Overall the bladder is pretty impressive. November is a time to recognize the bladder and different ways the bladder can be affected. We don't really think about how the bladder functions until something isn't functioning the way we want it to. So this month I am going to blurbs about the bladder and conditions that can change how the bladder functions. Let's begin with a crash course on the anatomy of how the bladder functions. The kidneys are connected to the bladder by ureters. The kidneys are responsible for filtering particles out of the urine before it passes to the bladder. The bladder functions as a storage unit for the fluid waste exiting your body. The bladder is hollow, it gets bigger as you drink. The bladder has a protective inner layer to protect it from the fluid inside. The muscles around the bladder and nervous system work together to store and release urine. The detrusor muscle surrounding the bladder relaxes to store urine and contracts to release urine. The detrusor muscle works with the urethral sphincters and pelvic floor musculature to properly release urine. The sphincters are circular openings surrounded by muscles, the muscles contract to close and relax to open. The bladder connects and empties into the urethra, the tube-like structure which allows for urine to leave your body. Now for men things are a little bit different as they have some extra anatomy around the urethra, the prostate. When the bladder becomes full it sends a message to the brain that it is full and needs to use the restroom. When the bladder sends the signal we make the conscious decision whether we want to use the restroom or put it off for a bit longer. So we have voluntary control over the bladder.
There you go! Now you have a summary on how the bladder functions! References: Image 1: https://courses.lumenlearning.com/ap2/chapter/gross-anatomy-of-urine-transport/ Image 2: http://slideplayer.com/slide/3408814/  Here in the United States we sit on toilets where are legs are at 90 degrees or even larger angles. Guess what? That is not the ideal position for having a bowel movement in fact, if you are already straining being in this position will only make having a bowel movement more difficult. We have a muscle in our pelvis, the puborectalis, that runs from the front of the pelvis back around the rectum and then connects back to the front of the pelvis again. It forms a sling basically. When we sit at a 90 degree angle this muscle cannot fully relax allowing the contents of the rectum to pass through as picture below on the left side. It's as if you take a garden hose and kink it slightly, the contents won't pass through as readily. The solution is to get into a squatting position. How do you do this? Have you heard of a Squatty Potty? If you haven't you need to add it to your Amazon wish list ASAP. In the picture on the right you can see how the position of the puborectalis and the colon changes with the squatting position (hips are both bent and the back is bent forward slightly--not hunched). The colon can more easily empty in this position without you feeling like you need to strain to empty your bowel. You can also use a stool to elevate your feet on the toilet to assume the squatting position, but I think the Squatty Potty is pretty nifty because it's the perfect height, comes in different sizes, plus it slides right under the toilet when you are done. Some other tips to avoid straining: 1. Try to relax when on the toilet. It does no good to sit there just pushing continuously. 2. Keep your mouth open when you are breathing so that you don't increase the pressure in your abdomen. 3. Give yourself enough time, about 10 mins. If you don't go in 10 minutes get up and walk around, try again at a later time. This may not apply to all individuals if you are concerned about your ability to have a pain-free bowel movement please see your local pelvic health physical therapist. |
AuthorHello! I am Caitlyn, Doctor of Physical Therapy and Board Certified Women's Health Physical Therapist working in St Louis, Missouri. Faculty in developing residency program. Endowarrior Categories
All
Archives
July 2021
|