Pelvic Health & Orthopedic Physical Therapy
Addressing your questions about pelvic, women's, and musculoskeletal health. Health is a journey. Movement is healing!
|
You went to the bathroom an hour ago, now you have to go again. In twenty minutes you will have to go to the bathroom once again. You will desperately need to find a restroom. Your life revolves around frequenting the bathroom to urinate, but when you go it doesn't always seem like all that much urine.
Does this sound like you? You may be experiencing the symptoms of overactive bladder. Individuals with this typically urinate more than eight times a day. When they do need to use the restroom, they are overcome with an intense urge to urinate. The urge make even lead to some urine leakage at times. When you do get to the restroom you quickly empty your bladder and head about your business, just to quickly rush back to the bathroom shortly. Why does this happen? Sometimes there is an underlying medical reason, other times we develop poor bladder health and train our bladder to go more often.So what can you do? A good first step if you suspect you have overactive bladder is to visit your physician. They can start medical management such as medications if necessary. You may also get referred to Physical Therapy to work on your pelvic floor muscles and retraining the bladder and your current bladder habits. Have you heard of painful bladder syndrome sometimes it's referred to as interstitial cystitis (IC)? It can be really tricky to diagnose so it could be years before getting diagnosed properly and receiving the right treatment. Some individuals just think they are continuing to get UTI’s even though the tests are negative. What is IC exactly? Even the definition is a bit tricky. The thought is interstitial cystitis is result of the lining of the bladder not functioning properly so the acidic contents of the bladder irritate the bladder wall. The body goes into an overdrive mode stimulating an inflammatory response and increasing the chemicals that make your body experience pain. The reason this occurs is not fully understood. Some studies point to genetic reasons, others say its root is in multiple bladder infections like UTI’s. When the organs have this reactions they have an effect on the musculature of the pelvic floor coupled with the pain that is experienced which leads to overactivity and tight musculature.
When the body develops this response it can either happen over a long amount of time or quickly. It is a painful syndrome, but can fluctuate in nature. So you will go through times of feeling okay and then times of intense pain. Pain is usually worse when you have a full bladder and is in the pelvic region primarily, but can occur elsewhere. You also may experience the need to get up during the middle of the night to use the bathroom. You might feel like you have to use the restroom more often or when you have to go you REALLY have to go! Pain may get worse around the time of your period. You may have pain with intercourse and following intercourse for a few days. If you feel like you are experiencing these symptoms and haven’t been treated the best place to start would to seek an appointment with a urologist or urogynecologist. They will run some tests to verify what is going on, help to get you on the correct medications, and possibly refer you to Pelvic Physical Therapy. There are a lot great websites out there with information. Here are just a few to start finding more resources. https://www.ic-network.com/ https://www.ichelp.org/ http://www.ic-today.com/ https://pelvicpain.org/home.aspx Do you ever laugh so hard a little pee just leaks out? Or maybe you are a cross-fit athlete and every time you do a lift you just leak a few drops. You just had a baby a few years ago and you never felt quite the same and now you notice when you gotta go to the bathroom you better start running or you end up with a little urine running down your leg. Maybe you constantly wear a pad or carry around extra panties due to fear of an accident.
Try as you might, you lose a little bit of pee, maybe it's even more than a small amount. This is called "urinary incontinence" when you unintentionally lose urine and there are a few different types. Stress Incontinence is when you accidentally lose pee. It can be with certain activities like coughing, sneezing, laughing, running, or when you stand up for sitting in a chair. These types of activities can change the pressure in your abdomen which influences your bladder and pelvic floor. If the muscles of your pelvic floor are weak they may have a difficult time staying closed to stop urine from coming down that urethra we talked about in the previous post. Urge Incontinence is when you accidentally lose urine with a strong urge to use the restroom. So you feel like you have to go to the bathroom and with the urge you lose control of your bladder and have a leak. The bladder has trained itself that it's time to go so you cannot wait. Oftentimes this is a mixture of pelvic floor musculature being both tight and weak. Functional Incontinence is when you physically cannot make it to the restroom so you have leakage. This could be that you are bed bound, unable transfer to the toilet on your own, or unable to unbutton your pants due to issues with dexterity in time causing loss in urine. So when does incontinence occur? Different types of incontinence can occur throughout different stages of life or with different conditions. Women commonly develop incontinence after giving birth and/ or after menopause. This can be due to the pelvic floor musculature going through changes as well as changes in hormones. And despite being told that this is "just old woman bladder" there is definitely techniques Physical Therapists can help you implement to better control your bladder. For men urinary incontinence and urgency can develop in individuals who have their prostate removed. 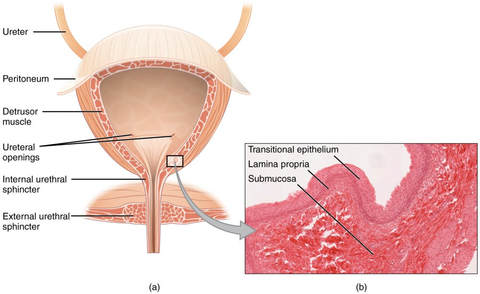 Overall the bladder is pretty impressive. November is a time to recognize the bladder and different ways the bladder can be affected. We don't really think about how the bladder functions until something isn't functioning the way we want it to. So this month I am going to blurbs about the bladder and conditions that can change how the bladder functions. Let's begin with a crash course on the anatomy of how the bladder functions. The kidneys are connected to the bladder by ureters. The kidneys are responsible for filtering particles out of the urine before it passes to the bladder. The bladder functions as a storage unit for the fluid waste exiting your body. The bladder is hollow, it gets bigger as you drink. The bladder has a protective inner layer to protect it from the fluid inside. The muscles around the bladder and nervous system work together to store and release urine. The detrusor muscle surrounding the bladder relaxes to store urine and contracts to release urine. The detrusor muscle works with the urethral sphincters and pelvic floor musculature to properly release urine. The sphincters are circular openings surrounded by muscles, the muscles contract to close and relax to open. The bladder connects and empties into the urethra, the tube-like structure which allows for urine to leave your body. Now for men things are a little bit different as they have some extra anatomy around the urethra, the prostate. When the bladder becomes full it sends a message to the brain that it is full and needs to use the restroom. When the bladder sends the signal we make the conscious decision whether we want to use the restroom or put it off for a bit longer. So we have voluntary control over the bladder.
There you go! Now you have a summary on how the bladder functions! References: Image 1: https://courses.lumenlearning.com/ap2/chapter/gross-anatomy-of-urine-transport/ Image 2: http://slideplayer.com/slide/3408814/ |
AuthorHello! I am Caitlyn, Doctor of Physical Therapy and Board Certified Women's Health Physical Therapist working in St Louis, Missouri. Faculty in developing residency program. Endowarrior Categories
All
Archives
July 2021
|