Pelvic Health & Orthopedic Physical Therapy
Addressing your questions about pelvic, women's, and musculoskeletal health. Health is a journey. Movement is healing!
|
It's October again. I know the hospital I work at is all decked out in pink. Awareness regarding breast cancer is everywhere. It's in the grocery store, there are races, it's even worked into the media. Awareness about the risk of developing breast cancer and celebration of survivorship are pretty apparent. Some of the struggles of survivorship are not as readily discussed. One issue that some women can face after treatment for breast cancer is perineal discomfort, urinary incontinence, and even pain with intercourse.
One of the biggest challenges for those navigating survivorship is things can be very overwhelming. There are a lot of financial, emotional, physical, and physiological impacts of fighting and surviving breast cancer that these individuals must face. It is sometimes difficult to find where physical intimacy and pelvic issues fit into the picture. Treatment for this type of cancer targets hormones in the body which can impact the tissues in the pelvic region. As a result discomfort, loss of urine, or pain with physical intimacy may occur. The muscles of the pelvic floor need estrogen and progesterone to function so by quickly removing them, the muscles don't know how to properly react. The muscles of pelvic floor may begin to develop weaknesses or areas of tenderness. The tissue integrity may change as a result of previous treatment. So when you are ready to seek treatment pelvic health physical therapy can help to address the changes that these tissues have experienced. With this type of PT they will look to restore improved tissue quality and provide the individual techniques for improved control over those muscles. They can provide insight on different lubricants and ways to decrease irritation from dryness. The PT can help to improve strength, muscle control, and decrease point tenderness. They can also help to trouble shoot different biomechanical difficulties occurring and help develop a plan to decrease accidental loss of urine. Everybody poops and according to Harris et al 2006 approximately 20% of individuals in the United States suffer from constipation. That's 1 in 5 people you meet have trouble pooping. So I've decided to do a series about constipation! Wohoo! So let's dive right in. It's not really surprising that so many people suffer from issues with constipation. I mean let's just think about some of the things that can contribute to constipation. DIET. We eat a lot of sugar, carbohydrates, and processed foods in America. You know how it feels a little like glue when you are chewing it? That's how it is in your gut as well. Pairing hand in hand with what we eat is what we drink. We don't get nearly enough water throughout the day. If we are lucky we stop to sip on water occasionally or some people avoid water altogether for more caffeinated and sugar-filled alternatives. But our gut needs water. The colon pulls all of the water out whatever is in it, so pair that with your gluey mess from above and you have something that just isn't going to budge very easily when you are sitting there on the toilet. Beyond diet there are some other factors that can contribute to constipation. Certainly the anatomy and motility of the intestines can play a role, but not every person walking around has had some change in the ability of their organs to move food through the digestive system (which is the definition of motility). So what else is there? Your pelvic floor muscles play a large role in the development and continuation of constipation. The muscles can become tight and can have a difficult time relaxing in order to have a bowel movement. Which is where a pelvic health or women's health physical therapist can come in to help alleviate your symptoms. The physical therapist can help to release those muscles, give you relaxation techniques, and then ultimately work on proper positioning and toileting techniques to help alleviate your symptoms of constipation. Symptoms of constipation can influence your overall health and well-being. They can cause you anything from mild to severe discomfort in your low back, abdominal, and perineal areas. I mean it just doesn't feel good when you can't have a bowel movement and you are all backed up. There are changes to diet and techniques physical therapists can help you to implement to offer relief from these symptoms. Stay tuned for part 2 on constipation we'll plunge a little deeper (pun definitely intended). References:
Harris LA, Hansel S, DiBaise J, Crowell MD. Irritable bowel syndrome and chronic constipation: Emerging drugs, devices, and surgical treatments. Curr Gastroenterol Rep. 2006;8:282–90. Sorry for the hiatus from blogging! I've been settling into my new place and job, things have just been a little bit on the crazy side. Anyways, lots has been going on.
So what's new? I recently went to another continuing education course on pelvic health physical therapy. We dove deeper into more complicated topics on gastrointestinal pathologies and pelvic pain. Remember all of those important muscles of the pelvic floor? They can impact your ability to have normal bowel movements. They have to lengthen for pleasurable intercourse. They also play an important role in a variety of pain diagnoses felt in the perineum, back, and legs. Chronic Pelvic Pain is described as pain in your pelvic region lasting longer for 6 months. The Mayo Clinic tweeted just this past week that 39% of women will experience Chronic Pelvic Pain at some point during their lifetime. This is just the number of women currently reporting their symptoms, so the number of women actually experiencing pelvic pain could be much larger. Many women just don't know who exactly to turn to for help. I just want to say that there are a lot of ways to help manage that pain and Pelvic Floor or Women's Health Physical Therapists can help patients with not only this type of pelvic pain, but many diagnoses. You see when our body experiences pain A) the muscles form a muscle memory and B) the muscles tighten and guard against the pain. If that pain stimulus does not subside our body continues to become more sensitive to pain triggers so smaller triggers elicit a greater pain response. This is true for ANY aspect of our body, including the muscles of the pelvic floor. So what does mean for an individual experiencing pelvic pain? A Pelvic Floor or Women's Health Physical Therapist can help you lengthen and relax your pelvic floor musculature, give you techniques to encourage more positive connections between the brain and muscles, and help to desensitize the area. After having a child, women in the United States return to their OB-GYN approximately 6 weeks after having a typical birth for a check-up. The physician performs an internal examination and check how you are healing from the birthing process. They may mention the importance of performing Kegel exercises or the issue of rehabilitation is skimmed over. At this point in time referring women to see a women's health or pelvic health PT following the birth of a child is not the standard of care in the US. It really should be. There are a lot of aspects of rehabilitation from birth that need to be managed (ie changes to pelvic floor structures). I mean think about it, birth is a huge process for a body to go through! A PT should be part of the team managing postpartum care with such a complex process that alters the musculoskeletal system. The pelvic floor is often overlooked in the recovery process and as a result down the road this can lead to urinary incontinence issues, prolapse, or issues with intercourse.
Now compare this to the model in other countries. In France after giving birth women are given up to 20 visits with a women's health PT to rehabilitate. It is also a common standard of care in the UK, Netherlands, as well as Australia to visit a "physiotherapist" (the equivalent of a Physical Therapist) for postpartum care. In the United States the Section on Women's Health (the professional organization representing the PT's treating women's health and pelvic health patients) is one of the smallest, but fastest growing physical therapy specialties. There still need to be more PT's in this specialty field in the US as in some parts of the country access to PT's practicing this specialty is limited. So what can you do? As a patient you can and should advocate for your healthcare. At your postpartum 6 week appointment with your OB-GYN you can ask your physician for a script to a women's health PT in your area to assess your rehabilitation needs. Don't be afraid to research what this postpartum PT care involves and talk to your physician about why you are interested in pursuing this care.
Chronic pain can be life altering. It is complex in nature with multiple variables and subtleties that contribute to it. Pain can be difficult to treat and manage. Women's health related pain conditions may require a myriad of Physical Therapy, medication, counseling, changes to diet, and other treatments.
There are a number of conditions that can cause pelvic pain. Here is a list of just a few examples:
A women's health PT can help you to manage pain related to many of these conditions. They can help to address the restrictions to the structures of the anatomy, educate you on self stretching, oscillatory exercises, massage, and techniques to properly engage your pelvic floor (just to name a few things). A women's health PT will help guide you through how to properly modulate your pain and give you techniques so that YOU are in control of your body. Sometimes the most frustrating part is finding the right practitioner to diagnose your pain or refer you to women's health PT if your state requires a referral to visit a PT. It can at times be an isolating experience for a patient if they feel their experience of pain is not being taken serious or properly addressed. Please rest assured that you are not alone. Many individuals experience pelvic pain, however, that does not normalize the pain. Pelvic pain is not a normal experience with urination, bowel movements, intercourse, sitting, exercise, using feminine hygiene products, or wearing pants. You should seek treatment. Just because you are a woman does not mean you have to grin and bear pelvic pain. I encourage you to utilize the Section on Women's Health PT Locator to find a PT near you if you are experiencing pelvic pain symptoms. They can help get you connected with the appropriate resources or schedule you for an evaluation.
http://www.womenshealthapta.org/pt-locator/
I've been reflecting a lot on transitions lately. With graduation quickly approaching (it's only TWENTY days away) there are a lot of exciting opportunities on the horizon. It also has me thinking on other transitions in life for people. One really big transition for the human body is giving birth, preparing to give birth, and then recovering from the birth process.
Your body goes through a lot of changes in order to prepare for birth. It produces a variety of hormones one of which is relaxin, a hormone that increases the laxity in your ligaments throughout your body. By increasing the laxity of your ligaments, your body makes it easier for the baby to pass through the pelvis, it can also alter the alignment of your sacroiliac joint. As the baby grows it changes your center of gravity. Essentially you are now carrying this growing basketball in the front of your abdomen as your baby grows it changes the way that forces are transmitted through your spine because it changes your posture in sitting, standing, and walking. This change in position and force in the spine can lead to back pain. As the baby grows it also changes the pressure on your abdominal and pelvic floor musculature as well as your bladder, it is constantly stretching these structures in order to make room. This can contribute to urinary frequency and urgency. Overall, your body is preparing to make space for your baby. A Women's Health Physical Therapist can help you to manage different musculoskeletal pain that arises during pregnancy as well as helping you to prepare for the birth of your child. Following childbirth those muscles and structures that were changed during pregnancy and the birthing process require time for rehabilitation. A Women's Health Physical Therapist can help to facilitate this process and return you to your baseline. Childbirth is a leading cause in developing urinary incontinence issues down the road so properly rehabilitating your pelvic floor as well as your back, hips, and abdomen following birth can be important in preventing symptoms of urinary frequency, urgency, and leakage. Yesterday I attended a course on physical therapy intervention with individuals who have survived urogenital and breast cancers. I continue to be amazed at the under utilization of pelvic rehabilitation by our medical system. A large portion of our population is aging. Age contributes to the risk of developing many types of cancer. As the baby boomer generation continues to age the number of individuals will continue to grow. Fortunately advances in medicine are improving the effectiveness of cancer treatments and increasing survivorship. The question for many physical therapists, especially women's health physical therapists, is when in this process of survivorship is it best to educate individuals on the availability of services?
While cancer treatment can be tailored to a specific region, the treatment can still have acute and chronic systemic effects. Chemotherapy can lead to pain, fatigue, as well as changes in bowel, bladder, and sexual function. Radiation can cause an individual to experience bladder changes, difficulties with the bowels, fibrosis of tissue, lymphedema, joint pain, fatigue, and difficulties with sexual function. (These are not exhaustive lists of the side effects of these types of treatments, just a few relevant to pelvic health.) There is evidence that physical therapy prior to treatment for cancer can play a beneficial role in post-treatment outcomes. Individuals that start improving physical shape before treatment often heal better. However, many insurance providers do not currently support "prehab". So the other options, target the individuals during or after treatment? There just doesn't seem to be a good time to address everything a survivor of cancer may face following treatment. Many individuals report feeling overwhelmed throughout the duration of treatment, which is understandable. Of course feeling constant diarrhea or bladder leakage or even changes in sexual function wouldn't necessarily be in the forefront of an individual's mind during treatment. These people are fighting to survive, which takes precedence. But then once they are discharged from cancer treatment, their needs beyond surviving cancer may fall between the cracks.They may even feel like they are the only one experiencing these symptoms or that there are no treatment options to help gain control of bowel, bladder, and sexual function. It is important to advocate and educate on pelvic health offerings along with other physical therapy services to help improve the quality of life. Regardless if you treat pelvic floor specifically, you will most likely have a cancer survivor as a patient and it is crucial to ask pertinent questions related to bladder, bowel, and sexual function in order to connect patients with appropriate resources. 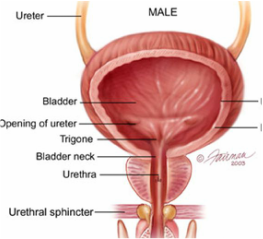 Male Bladder Anatomy Male Bladder Anatomy Well it seems like time is passing exceptionally quickly this year. It is already NOVEMBER. November is prostate cancer awareness month or more affectionately called Movember. So wear your facial hair proudly and promote support and awareness of prostate cancer. As such, I thought I would do a run down of prostate health, prostate cancer, and physical therapy rehabilitation following the removal or reduction of the prostate. Just a quick anatomy lesson. The prostate is a gland in the male body that surrounds the urethra at the base of the bladder. It is part of the male reproductive system. Just below the prostate lies the pelvic floor musculature that controls the opening and closing of the urethra and supports the internal organs. As men age their prostate grows in size. This cell growth can be benign in nature, which is oftentimes referred to as BPH (Benign Prostate Hyperplasia). When there is growth in the prostate gland it may make it more challenging for an individual to pass urine. However, with increased age also comes the increased chance that the cell growth in the prostate gland becomes cancerous. One in seven men will develop prostate cancer during his lifetime. It is the second most common cancer in men over the age of 65 years old. Men are encourage to seek examinations of their prostates starting at age 50 to monitor the development of prostate cancer. The symptoms for prostate cancer are similar to that of an enlarged prostate (BPH) including: difficulty passing urine or emptying the bladder, increased frequency to pass urine, pain with urination, pain or difficulty with intercourse. These symptoms may also present with pain in the back, hips, and abdomen. Talk to your physician if you are experiencing any of these symptoms. So how does this relate to physical therapy? Following medical intervention to treat prostate cancer or BPH men may begin to experience symptoms on the other end of the spectrum, they accidentally lose control of their bladder and experience urinary leakage. If you look at the picture of the male bladder anatomy above, just below the prostate is the urethral sphincter, which is composed of musculature that controls the opening and closing of the urethra. For so long the prostate regulated the flow or rather lack of flow of urine so the pelvic floor musculature may have become weak and/or uncoordinated or previous insufficiency with this musculature is finally unmasked. The pelvic floor is now the primary regulator for passing urine and if it is weak or uncoordinated the chance of unexpectedly or accidentally urinating increases. Physical Therapists with specialized training in pelvic floor rehabilitation can identify this pelvic floor dysfunction and help an individual strengthen and gain control over their pelvic floor, allowing the individual to control urination. "Am I the only one who has this?" So many individuals who experience pelvic health issues ask this question. They fear that they are the only person with urinary leakage, fecal incontinence, constipation, pelvic pain....the list goes on. The answer is no, pelvic floor dysfunction is more common than you think.
Men, women, and children are all susceptible to developing issues with their pelvic floor musculature. Muscular imbalances, soft tissue abnormalities, and misalignment in joints can alter the pelvic floor and impact an individual's ability to control their bowel and bladder as well as manage pain associated with the pelvic floor muscles. Women have a higher risk of developing issues with their pelvic floor. This risk is increased with hormone fluctuations, age, and giving birth. In fact in 2010, it was estimated that 28.07 million women in the U.S. over the age of 20 experienced some form of pelvic floor dysfunction. This number is estimated to increase to 31.88 million women over the age of 20 by the year 2020 experiencing pelvic floor dysfunction according to Herman & Wallace. So no, you are definitely not the only person with your symptoms. It is more common than you think. Not only are your symptoms more common than you think, but there may be a non-pharmaceutical treatment for your symptoms with pelvic or women's health physical therapy. The incidence of pelvic floor dysfunction in men and children is lower. However, for men, it increases post-prostatectomy. Bowel, bladder, and reproductive function may feel uncomfortable to talk about, especially when you are experiencing an issue. Rest assured you are not the only one with theses symptoms. Just walk down the feminine care isle or turn on the TV there are lots of products and medications available to manage your symptoms. These products will not fix the muscular dysfunction that may cause your symptoms, but physical therapy can help address these deficits. Talk to your physician or Physical Therapist about seeking the services of a pelvic or women's health physical therapist.  So my next clinical experience is in outpatient orthopedics and pelvic floor therapy (sometimes referred to as "Women's Health"). I don't think many people realize that there are Physical Therapists who are qualified to treat pelvic disorders. I'll save the reasons for my interest in learning more about this field of therapy for a different blog post. Instead let me tell you more about my past weekend. Last weekend I attended the SOWH's Pelvic Floor Physical Therapy Level I class in St. Louis. I did not know what to fully expect and while I was excited for the course, I was extremely apprehensive for the lab portions. What I did not expect was for my fears to be assuaged so quickly and to feel so empowered from the action-packed three day course. We really hit the ground running. Physical therapy is a broad field. One component of the body people are often uncomfortable confronting is the pelvis. In our culture it seems taboo to bring up disorders related to the pelvic region, but let me let you in on a little secret....everybody has a pelvis. That pelvic region is made up of many bones, nerves, arteries, veins, lymphatics, organs, ligaments, and muscles that serve very important roles. The pelvis region helps to transmit forces for the legs to spine or vice versa, the pelvic musculature/bones/ligaments offer a bowl like support to all organs, the musculature of the pelvic floor can alter your ability to appropriately excrete waste. The bony pelvis and the musculature that makes up this pelvic floor is a keystone to our anatomy, serving many important purposes, yet we oftentimes ignore the treatment of this area because we don't fully understand it or it is uncomfortable to treat. Let's embrace this crucial part of our anatomy. Personally, I think that people are oftentimes apprehensive about seeking treatment for pelvic issues. Pelvic Floor or Women's Health Physical Therapists are specially trained to deal with incontinence, organ prolapse, pelvic pain, and constipation, just to name a few of the common diagnoses. And while it may be a bit misleading Women's Health Physical Therapists oftentimes also take male patients and children with pelvic floor issues. Women's Health therapists may actually treat a lot of different types of patients and diagnosis (not just related to the pelvis) including patients with breast cancer, patients before or after having a child, patients with fibromyalgia, patients requiring lymphedema management...the list really does go on and on. You might be thinking, I already know how to do Kegel (pronounced like kay-gal) exercises, I don't need to see anyone about that. Kegel exercises are important to the integrity and control of the pelvic floor musculature. If you are having pelvic floor related issues, it would be of benefit to have a PT ensure you are doing your Kegel exercises correctly (that you have the right form, you have enough power with the contraction, can properly perform this exercise as an endurance exercise). Beyond that there is so much more to rehabbing these individuals than just prescribing Kegel exercises. It really is just the tip of the proverbial iceberg. Issues in your pelvic floor musculature could be a result of postural abnormalities or muscular imbalances in other areas of the body that are manifesting as pelvic symptoms because they altered the integrity of the pelvic floor. Depending on the symptoms/ diagnosis there are hormonal and behavioral interventions that must be addressed in order to properly rehabilitate the pelvic floor musculature. There are many considerations for appropriate treatment. Bottom line, as a student in Physical Therapy school I really appreciated the continuing education course. I thought it was a great way to learn more about a subject we learn very little about in school. It was a fantastic way to prepare for my upcoming clinical and gain new clinical skills. It also allowed me to network with other PT students and many practicing PTs. This class made me excited to attend more courses, especially those pertaining to Women's Health. |
AuthorHello! I am Caitlyn, Doctor of Physical Therapy and Board Certified Women's Health Physical Therapist working in St Louis, Missouri. Faculty in developing residency program. Endowarrior Categories
All
Archives
July 2021
|